
Hypoglycemia The First Step In Recovery
Hypoglycemia is a problem for those trying to recover and can be contributing to your fatigue. Hypoglycemia is a stress on the body and this stress could be delaying your recovery.
What is hypoglycemia?
Hypoglycemia is low blood sugar. A variety of symptoms might present when your glucose (blood sugar) level falls too low. Symptoms include irritability, dizziness, sweating, brain fog, and agitation.
Blood sugar regulation is often a problem in people with Chronic Fatigue Syndrome (CFS), mitochondrial dysfunction, HPA axis dysfunction / adrenal insufficiency, and or metabolic inflexibility.
How Does Blood Sugar Regulation Work?
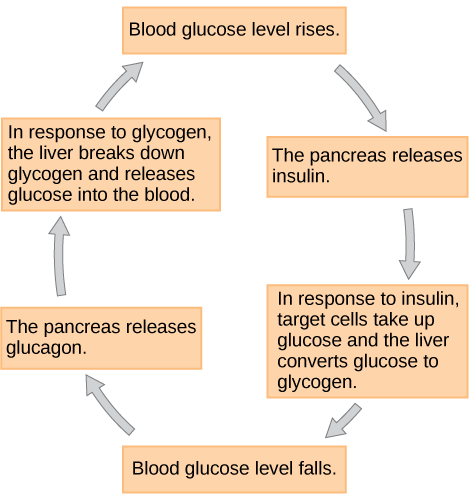
Glucose is an essential energy source for your body, your brain needs glucose to function. When glucose rises your pancreas releases insulin that allows the glucose to enter the cells and to provide the fuel your cells need to function. Excess glucose is stored in the fat cells, liver, and muscles in the form of glycogen. Your blood sugar rises after you eat and will decrease the longer you go without food. After a couple of hours of not eating and your glucose drops to a certain level your pancreas releases glucagon which sends a message to your liver to breakdown the stored glycogen and releases glucose back into the bloodstream. This keeps your blood sugar in a healthy range until you eat again.[1]
Because people with chronic fatigue usually have some form of HPA axis dysfunction, insulin resistance, and/or lack of metabolic flexibility this results in problems with blood sugar regulation which leads to episodes of hypoglycemia.
What does Hypoglycemia look like?
Symptoms can include:
- Dizziness
- Sweaty feet/palms
- Hunger
- Agitation
- Low blood pressure
- Trouble thinking
- Pale skin
Why is hypoglycemia a problem in those with Chronic Fatigue Syndrome?
People with CFS have trouble regulating blood sugar. Some people can have high levels others can have low. Low blood sugar is often caused by sub-par adrenal function or HPA axis dysfunction, insulin resistance, and liver function.
Liver and HPA Axis Role in Blood Sugar Regulation
The liver controls blood sugar by releasing sugar energy stores into the bloodstream. Eating too many refined carbohydrates or sugar can overwhelm the liver’s ability to regulate blood sugar resulting in the body to be flooded with too much sugar and there isn’t enough activity to burn off the energy. As a result, the pancreas excretes insulin and the insulin brings blood sugar levels down by shunting the sugar into the fat.
Additionally, if you are fighting an external environmental toxin like mold this will be adding further work to you liver and could be impairing blood sugar regulation.
With an improperly functioning system, too much insulin can be excreted by the pancreas which in turn drops the blood sugar level too low resulting in hypoglycemia. This triggers a stress response in the brain. In order to boost the blood sugar levels back up the HPA axis kicks in where the adrenal glands secret cortisol into the liver to be converted to glucose. The hypothalamic-pituitary-adrenal (HPA) axis activity plays a critical role in the counterregulatory response to hypoglycemia. This is why preventing hypoglycemic episodes is important to improving HPA Axis functioning.
When your blood sugar drops you are likely to feel unwell. Shaky, dizzy, agitated and as a result you reach for sugar or carbohydrates to feel better. Thus repeating the cycle all over again. It becomes a roller coaster. As you can probably tell by now, recurrent episodes of hypoglycemia are very taxing on the liver and adrenal glands .
Hypoglycemia is a stressor for those with Chronic Fatigue Syndrome and one of the goals in recovery is to eliminate stress, both physiological and psychological.
Emotional Stress
If you are not eating a lot of sugar stress can also be the cause of hypoglycemia. This is why the Chronic Fatigue Protocol addresses both a mitochondria problem and a nervous system problem. When we have a fight or flight response many hormones are released. One of them is insulin which will cause a drop in blood sugar. Therefore, hypoglycemia can be both a result of stress and a cause of stress. Any hypoglycemic episode is a stressor on the body (liver and adrenals).
In a healthy body when blood glucose levels fall glycogen stores in the liver are mobilized to increase the blood sugar. The problem is that glycogen stores are probably low is someone who is not well. Another way to boost blood sugar is when the liver converts short-chain fatty acids into glucose. Short-chain fatty acids are made in the gut by bacteria fermenting fiber. If you have a poor diet or poor gut function your conversion by short-chain fatty acids may be suffering.
Short-Chain Fatty Acids
Short-chain fatty acid deficiency might also explain why you are shooting awake between 2 am and 3 am. Blood sugar falls in the middle of the night and if there aren’t sufficient short-chain fatty acids then you will be jolting awake in the middle of the night because your blood sugar had dropped. Your body produces adrenaline to bring your blood sugar back up thus, jolting you awake.[2]
How to Fix it?
First, we must adjust the diet and eat foods that reduce hypoglycemia and insulin resistance. The first step is to eat low glycemic index foods. This means avoiding foods containing sugar and refined carbohydrates. Once the body is experiencing episodes of hypoglycemia it may take weeks or months for the liver to be able to stabilize the blood sugar, so this will take some time. This means when you make this shift you will not necessarily notice an immediate change you will still experience some episodes but sticking to the process with balance the liver over time.
Second, increase the consumption of healing foods that rebuild the body and reduce inflammation. Increase protein, vegetables, and healthy fats. Eliminate high inflammatory foods such as processed food, gluten, dairy, and sugar. Think of this as a modified Paleo diet.
Essentially you are going to cut out wheat, sugar, and dairy. Your carbohydrate intake will consist of complex non-inflammatory carbs sweet potatoes, quinoa, rice. You will increase your protein, vegetable, and healthy fat intake to balance out the calorie reduction from eliminating wheat, processed carbs/food, and sugar.
Eat regularly, every 2.5-3 hours:
To start you should eat regularly every 2.5-3 hours. Going longer than this could result in a drop in blood surgar and will trigger the stress cycle. Over time you will be able to lengthen the duration of when you need to eat, but to start the goal is to eliminate the blood sugar rollercoaster.
- Breakfast (within one hour of waking) 6:30-8
- Snack 10-1030
- Lunch 12:30-1:00
- Snack 3:00-3:30
- Dinner 5:30-60
- Snack 8-8:30
Note: if you feel your blood sugar drop the reaction is to boost it quickly consuming a lot of carbs. Try and lower the dose of sugar you need to remedy the hypoglycemia. For example if you would grab an apple when your blood sugar drops in stead of eating the whole apple only eat half. See how you feel after a little while. Half may have been all you needed to get out of the crisis. Over time you will reduce the amount of sugar you need to get out of crisis mode.
Foods to Add
- Protein (Grass-fed meats, pasture meat, wild caught fish)
- Healthy Fats (Avocado, Olive Oil, Coconut Oil, Butter)
- Vegetables
- Fiber
- Resistance Starch (cold white rice, green bananas)
- Complex Carbohydrates (Quinoa, Soaked Beans, Sweet Potato)
Foods To Eliminate
- Wheat
- Sugar
- Dairy
- Alcohol
- Caffeine
Supplements
- Multi-vitamin with trace minerals (I find the best supplement is organ meat pills)
- Vitamin C (for adrenal support)
- Magnesim
- B Vitamins
- Essential Amino Acids
- Salt
Tips:
- If you are experiencing a crash try avoiding consuming a lot of sugar. When you crash, eat just a little bit to see if it helps. Overtime by eating more frequently and increasing salt intake your blood sugar levels will balance out and you won’t be experiencing the hypoglycemic crash.
- Drink essential amino acids to get more protein and help stabilize your blood sugar throughout the day
- Drink salt water, or add salt to your food to increase blood volume.
- Drinking saltwater in the morning helps support the adrenals in the morning.
- If health allows, try walking after you eat to improve insulin resistance and the glucose response.
Sources:
[1] Mayo Clinic Hypoglycemia [Back To Text]
[2] Hypoglycemia (Low Blood Sugar) – A Problem For Many Chronic Fatigue Syndrome And Fibromyalgia Patients, But Treatable [Back To Text]
